Table of Contents
- Understanding Wheelchair Insurance Basics
- Key Concepts in Wheelchair Insurance
- Benefits of Proper Wheelchair Insurance Coverage
- How Wheelchair Insurance Processes Work
- Best Practices for Securing Wheelchair Insurance
- Securing Mobility Through Insurance
Understanding Wheelchair Insurance Basics
At MedEquipped, we understand that wheelchair insurance plays a vital role in helping individuals with mobility challenges access the custom motorized wheelchairs they need. Whether you’re navigating coverage in New York, Georgia, or Michigan, securing the right financial support can make all the difference in achieving greater independence and comfort in daily life. As your partner in mobility freedom, we simplify this process from start to finish.
Wheelchair insurance typically refers to financial support for durable medical equipment like power wheelchairs, covering sources such as Medicare wheelchair coverage, Medicaid, and private insurers. For Medicare, eligibility hinges on medical necessity, requiring a face-to-face examination and written prescription from your provider to qualify. We handle the paperwork, insurance navigation, and coordination, using our certified ATP-led evaluations to justify needs for models like the QUICKIE series or ROVI X3. This often leads to wheelchair insurance reimbursement after meeting deductibles, with patients paying about 20% of approved costs. Our end-to-end services, including clinical fittings and funding assistance, streamline approvals on a faster 30-60 days timeline, as seen in cases like a Michigan patient who received their custom chair without hassle.
In the sections ahead, we’ll dive deeper into coverage details, benefits, application steps, and best practices tailored to your region. Stick with us to learn how we can support your power wheelchair financing options and ensure you get the mobility aid funding that fits your life.
Key Concepts in Wheelchair Insurance
At MedEquipped, we understand that navigating wheelchair insurance can feel overwhelming, but grasping the key concepts empowers you to access the right mobility solutions. We specialize in guiding patients through coverage for custom power wheelchairs like the TDX SP2 HD, handling everything from evaluations to approvals. This section breaks down essential ideas to help you see how insurance opens doors to greater independence.
Types of Coverage for Power Wheelchairs
Wheelchair insurance plays a crucial role in making advanced mobility equipment affordable. We often see patients relying on Medicare, Medicaid, or private plans to cover custom models from the QUICKIE series, which are designed for specific needs like heavy-duty support or precise controls.
Medicare Part B serves as a primary source of medicare wheelchair coverage, paying 80% of the cost after your deductible for durable medical equipment (DME) that’s deemed medically necessary. According to CMS guidelines, this includes power wheelchairs if a physician confirms they’re essential for daily activities. Medicaid, a state-federal program, offers DME insurance options tailored to low-income individuals, often providing full coverage for items like the ROVI X3 when justified by clinical evaluations. Private insurance varies by policy but frequently mirrors Medicare, covering upgrades or custom features with co-pays based on your network.
These options highlight power mobility funding pathways, ensuring patients get fitted chairs that enhance their lifestyle. We at MedEquipped partner with you as a partner in mobility freedom, coordinating claims to simplify the process.
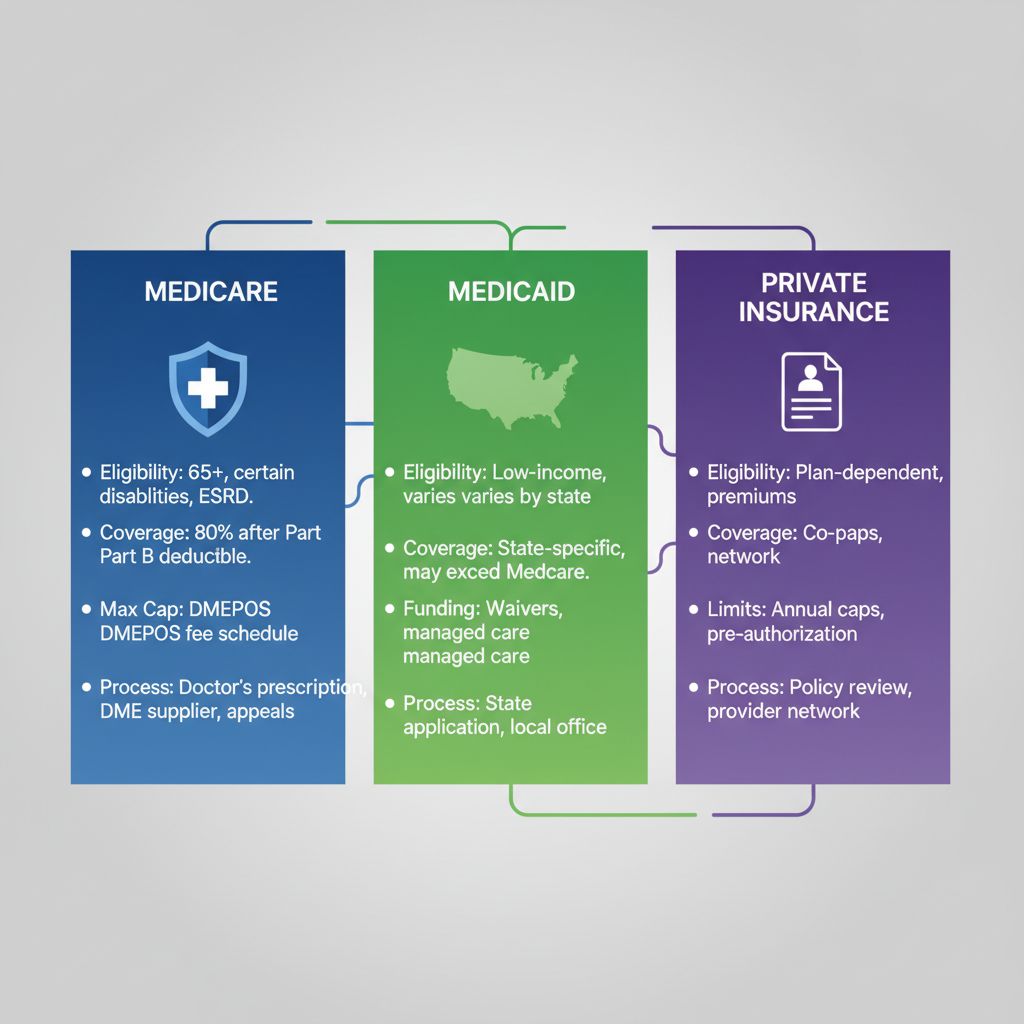
The following table provides an overview of wheelchair insurance types, comparing key aspects to clarify how each might apply to your situation:
| Coverage Type | Eligibility Criteria | Coverage Limits | Application Process |
|---|---|---|---|
| Medicare Part B | Covers 80% after deductible for medically necessary equipment | In-home assessment required | Supplier handles prior authorization |
| Medicaid | Varies by state, often full coverage for low-income | State-specific documentation | Coordination with state programs |
| Private Insurance | Policy-dependent, often similar to Medicare | Co-pays and networks apply | Claims submission required |
This comparison shows Medicare’s structured approach versus Medicaid’s flexibility for underserved groups, while private plans add personalization. At MedEquipped, we streamline applications across these types, leveraging our expertise to boost approval rates and reduce wait times to our typical 30-60 days. By aligning your needs with the right coverage, we help secure custom motorized wheelchairs that fit seamlessly into your life.
Building on these coverage basics, let’s explore how eligibility ties into getting the equipment you need. Our team often assists with documentation to meet these standards, ensuring a smoother path forward.
Eligibility and Medical Necessity Requirements
Securing wheelchair insurance reimbursement starts with proving medical necessity, a step we at MedEquipped guide you through every time. A physician’s certification is essential, typically including a face-to-face exam and a detailed letter of medical necessity outlining why a power wheelchair improves your function and quality of life.
Functional assessments, like those conducted by our certified Assistive Technology Professionals (ATPs), evaluate mobility limitations and recommend specific features. Drawing from the assistive technology funding guide, these evaluations align with insurer requirements, such as documenting how the chair addresses impairments in ambulation or daily tasks. Common criteria include:
- Inability to use a manual wheelchair or cane independently due to conditions like muscular dystrophy or spinal cord injury.
- Home and community mobility needs that standard walkers can’t meet.
- Physician orders specifying the model, like the QUICKIE for lightweight versatility.
We handle the paperwork, insurance navigation, and coordination to compile these elements, often speeding up approvals. Remember, results may vary, and we recommend consulting your healthcare professional for personalized advice. This thorough process ensures your custom motorized wheelchair meets DME standards and supports long-term independence.
Regional Variations in New York, Georgia, and Michigan
While core wheelchair insurance principles remain consistent, regional differences across our service areas in New York, Georgia, and Michigan add important nuances, especially for Medicaid processes. In Michigan, the Department of Health and Human Services (DHHS) oversees robust DME reimbursements, with prior authorizations required for complex items like power wheelchairs. Their guidelines emphasize ATP evaluations and state-specific forms, often covering full costs for eligible low-income residents; Medicaid wheelchair insurance here approves custom bases if documentation shows necessity.
New York and Georgia share similarities, such as income thresholds for Medicaid and alignment with federal Medicare rules, but Michigan stands out for its detailed fee schedules and liaison meetings for providers. For instance, Michigan’s DMEPOS database lists codes for models like the TDX SP2 HD, facilitating faster claims. Across all states, private insurance follows policy networks, but state Medicaid waivers can expand options for specialized seating.
We at MedEquipped navigate these variations seamlessly, from New York’s urban delivery logistics to Georgia’s rural access needs and Michigan’s reimbursement protocols. By understanding local rules, we maximize your coverage and deliver ongoing support, helping you focus on mobility rather than bureaucracy.
Benefits of Proper Wheelchair Insurance Coverage
At MedEquipped, we understand how vital wheelchair insurance can be for accessing the mobility solutions you need. As your partner in mobility freedom, we help patients navigate coverage to unlock financial relief, advanced options, and ongoing support across New York, Georgia, and Michigan. Proper coverage transforms challenges into opportunities for independence, ensuring custom motorized wheelchairs fit your life without overwhelming costs.
Financial Relief and Reimbursement Advantages
Securing wheelchair insurance provides essential financial relief by minimizing out-of-pocket expenses for high-quality power wheelchairs. Through our expertise, we handle the paperwork, insurance navigation, and coordination to maximize reimbursements, often covering 80-100% of equipment costs. For instance, Michigan Medicaid DME reimbursement offers robust funding for durable medical equipment in that state, with successful claims averaging significant savings as noted in our reimbursement FAQ resources.
Wheelchair insurance reimbursement processes streamline access to funding for powered wheelchairs, reducing the burden on patients. Medicare wheelchair coverage, for federal benefits, supports eligible individuals with medically necessary devices, while state programs enhance these options. We assist with documentation to expedite approvals, helping families avoid unexpected bills. Key advantages include:
- Coverage for custom features that standard plans might overlook.
- Reduced financial stress, allowing focus on health and daily activities.
- Integrated support for both private insurance and public programs like Medicaid.
This approach not only safeguards your budget but also ensures timely access to essential mobility aids, with processing typically in 30-60 days for faster relief.
Access to Advanced Mobility Solutions
Wheelchair insurance opens doors to advanced mobility solutions, enabling personalized access to models like the ROVI X3 that match your unique needs. Our certified Assistive Technology Professionals (ATPs) conduct evaluations to recommend insurance-backed mobility aids, ensuring coverage aligns with clinical requirements. In states like New York, Georgia, and Michigan, this means faster delivery timelines and custom fittings without delays.
With proper coverage, patients gain entry to heavy-duty bases and tailored controls, enhancing safety and independence on various terrains. We help secure funding for powered wheelchairs through Medicare wheelchair coverage and state initiatives, quoting coverage rates up to 90% for complex devices from our Medicaid details. This support reduces wait times from industry standards, often fulfilling orders in 30-60 days.
Benefits extend to health improvements, as timely mobility aids prevent secondary issues like pressure sores, affecting up to 60% of users without proper support. We prioritize these outcomes daily, integrating education on device use. Advantages include:
- Personalized seating for optimal posture and comfort.
- Access to premium brands with advanced joystick options.
- Streamlined approvals for lifestyle-specific customizations.
By leveraging insurance, you unlock solutions that empower greater freedom.
Long-Term Support and Adjustments
Beyond initial acquisition, wheelchair insurance delivers long-term support for repairs, adjustments, and education, sustaining your mobility investment. At MedEquipped, our post-delivery services in New York, Georgia, and Michigan include routine check-ins and ATP-led modifications, often covered under existing plans. This ongoing care ensures devices remain effective as needs evolve.
Medicaid wheelchair insurance perks, particularly in Michigan, bolster durable medical equipment funding for maintenance, with high coverage rates for eligible patients. We coordinate wheelchair insurance reimbursement for these services, drawing from successful claim examples in our FAQs to illustrate sustained savings. This holistic approach addresses real-world changes, like terrain adaptations or control tweaks.
Our team provides caregiver training and pressure mapping to promote safety, preventing common issues. As a partner in mobility freedom, we handle follow-ups to maintain performance. Key benefits encompass:
- Covered repairs for wear and tear on custom components.
- Adjustments for changing health conditions without extra costs.
- Educational resources for independent use and longevity.
These elements preview the application steps we’ll cover next, where securing coverage unlocks these enduring advantages. Results may vary; consult a healthcare professional for personalized advice.
How Wheelchair Insurance Processes Work
Navigating wheelchair insurance can feel overwhelming, but at MedEquipped, we partner in mobility freedom by handling the details for you. Our team guides patients through every stage, from initial assessments to final delivery, ensuring smoother access to custom motorized wheelchairs. We focus on power wheelchairs, though processes for manual wheelchairs follow similar steps.
Initial Evaluation and Documentation
The journey begins with a physician referral, where your doctor assesses your mobility needs and determines if a power wheelchair is medically necessary. This step proves the device’s role in improving daily independence, much like manual wheelchairs for lighter needs. At MedEquipped, our certified Assistive Technology Professionals (ATPs) conduct a comprehensive clinical evaluation, including face-to-face exams and home assessments to match equipment to your lifestyle in New York, Georgia, or Michigan.
Wheelchair insurance requires detailed documentation, such as medical necessity forms outlining your condition and functional limitations. We handle this paperwork, coordinating with your physician to compile reports that highlight how the device addresses specific barriers. Common pitfalls, like incomplete forms, can delay approval, so our ATP process ensures thorough, accurate submissions from the start. This evaluation phase typically takes 1-2 weeks, setting a strong foundation for your mobility funding application.
In Michigan, for instance, state-specific eligibility checks add another layer, but we streamline it all. By proving necessity upfront, we position your claim for success under programs like Medicare wheelchair coverage, reducing overall wait times.
Submission and Approval Steps
Once documentation is ready, we submit your application to the insurer, initiating prior authorization for wheelchair insurance reimbursement. This involves uploading physician orders, ATP reports, and supporting evidence to Medicare or Medicaid portals. For federal steps, Medicare wheelchair coverage demands clear proof of medical necessity, often reviewed by durable medical equipment suppliers like us.
Variations exist between programs, as shown in the table below, which compares key timelines based on CMS guidelines and Michigan DHHS processes.
| Step | Medicare | Medicaid (Michigan Focus) |
|---|---|---|
| Evaluation | Face-to-face exam + ATP report (1-2 weeks) | State eligibility check (1 week) |
| Submission | Prior auth via supplier (2-4 weeks) | Coordination with MedEquipped (2-3 weeks) |
| Approval to Delivery | 30-60 days total | Similar, with state variations (30-60 days) |
Medicare often moves faster for straightforward cases, while Medicaid in Michigan requires extra coordination for state funding, including appeals if initial denials occur. We manage these insurance claim procedures, tracking submissions and addressing queries to avoid delays. Average approval takes 2-4 weeks for prior auth, but our expertise shortens the full process to our standard 30-60 days timeline.
If issues arise, we assist with appeals, drawing from common FAQ insights like ensuring all certificates of medical necessity are complete. Our end-to-end handling means you focus on recovery while we navigate the bureaucracy.
Delivery and Post-Approval Support
Approval unlocks custom ordering, where we configure your power wheelchair with features like tilt-in-space or specialized seating for optimal comfort. We then arrange delivery directly to your home in New York, Georgia, or Michigan, complete with professional fitting by our ATPs to ensure proper setup and safety.
During delivery, we provide hands-on training on controls, maintenance, and daily use, empowering you to maximize independence right away. This session covers troubleshooting basics, so you feel confident from day one.
Post-delivery, our ongoing support includes follow-up adjustments, repairs, and check-ins to adapt the chair as your needs evolve. We handle warranty claims and any insurance-related tweaks, maintaining your mobility solution long-term. With MedEquipped, we go beyond delivery to build lasting partnerships in your journey toward greater freedom.
Best Practices for Securing Wheelchair Insurance
Securing funding for a power wheelchair can feel overwhelming, but with the right steps, you can streamline the process and achieve mobility freedom faster. At MedEquipped, we partner in mobility freedom by handling the paperwork, insurance navigation, and coordination to help you obtain custom motorized wheelchairs efficiently. Our certified Assistive Technology Professionals (ATPs) guide you through every stage, aiming for our typical 30-60 days processing timeline. Follow these best practices to optimize your insurance claims and improve approval chances.
Preparing Documentation and Evaluations
Start your journey toward wheelchair insurance by gathering comprehensive records early. We recommend consulting your physician promptly to obtain a detailed prescription outlining your medical needs and how a power wheelchair enhances your independence.
- Collect Medical History: Assemble recent doctor’s notes, diagnostic reports, and therapy evaluations that demonstrate your mobility limitations. This builds a strong case for medical necessity.
- Leverage ATP Assessments: Schedule an evaluation with a RESNA-certified ATP like those on our team. These professionals perform in-depth seating and mobility analyses, including pressure mapping to prevent issues like skin breakdown, which affects up to 60 percent of users without proper support. Their reports justify the need for customized features.
- Include Supporting Evidence: Add photos of your current mobility challenges and lifestyle details to personalize your application. For integrated solutions, consider services like orthotics near me to complement your wheelchair setup.
By preparing thoroughly, you’ll strengthen your wheelchair insurance application and reduce delays. Our experts can assist with documentation to ensure everything aligns with insurer requirements.
Navigating State-Specific Requirements
Insurance rules vary by location, so tailor your approach to your state’s guidelines. For federal options, explore medicare wheelchair coverage, which treats power wheelchairs as durable medical equipment when medically necessary. We handle these details to simplify reimbursement.
In Michigan, Medicaid requires proof of income and residency, along with a physician’s certification of need. Submit forms like the MA-1021 for prior authorization, including ATP evaluations for complex cases. Contact your local Medicaid office early to confirm eligibility checklists.
For residents in New York, Georgia, and Michigan, we offer targeted support. Reach out to us at 845-237-2381 for intake—we coordinate wheelchair insurance reimbursement across these states, from virtual screenings to full paperwork submission. Effective funding strategies include bundling state grants with insurance for broader coverage.
Our streamlined process ensures compliance, helping you navigate requirements in Michigan or elsewhere without hassle.
Common Pitfalls and How to Avoid Them
Even strong applications can face hurdles, but proactive steps minimize risks. One common issue is incomplete documentation; always double-check for missing signatures or outdated records to avoid denials.
If an appeal is needed, respond within the 30-day window with additional ATP insights or physician letters. We guide you through resubmissions, drawing on our experience with successful reversals.
Explore alternatives like VA funding for veterans or low-interest loans if primary insurance falls short. Post-approval, maintain coverage by scheduling regular check-ins—our ongoing support includes in-home adjustments and caregiver education to prevent lapses.
Timely submissions keep you on track for 30-60 days fulfillment. By avoiding these pitfalls, you’ll secure lasting access to your custom power wheelchair and sustained mobility support.
Securing Mobility Through Insurance
Navigating wheelchair insurance can unlock vital mobility solutions, ensuring access to devices that enhance daily life. From understanding medicare wheelchair coverage to exploring wheelchair insurance reimbursement options, the path to funded mobility involves verifying medical necessity through a face-to-face exam and prescription, as outlined by Medicare Part B. This coverage typically applies after meeting the deductible, with patients paying 20% of approved costs for durable medical equipment like power wheelchairs. While manual wheelchairs manual wheelchairs offer basic support, advanced models such as the QUICKIE series or TDX SP2 HD provide customized power assistance for complex needs, often covered when deemed essential for independence.
At MedEquipped, we serve as your partner in mobility freedom, offering end-to-end services in New York, Georgia, and Michigan. Our certified Assistive Technology Professionals (ATPs) conduct thorough evaluations, handle the paperwork, insurance navigation, and coordination, and deliver custom motorized wheelchairs within our faster 30-60 days processing timeline. We streamline insurance-enabled access, from initial assessments to post-delivery support, ensuring long-term comfort and adjustments.
Ready to take the next step? We’re here to help with personalized consultations. Reach out at intake@medequipped.com or call (845) 237-2381 to discuss your options and achieve greater independence today.
Resources
- Discover Lightweight QUICKIE Manual Wheelchairs for Easy Mobility
- Explore Ultra-Lightweight QUICKIE Wheelchairs for Independent Mobility
- Get Custom Orthotics Integrated with Power Wheelchairs
- Obtain Professional ATP Wheelchair Fitting Services
- Start Custom Orthotics Process with ATP Evaluations
- Find Advanced Wheelchair Seating Systems for Posture Support
- Schedule RESNA-Certified Wheelchair Fittings in Georgia
- Learn Medicare Coverage for Wheelchairs and Scooters
- Explore Funding Resources for Assistive Technology Devices
- Access Michigan Medicaid DME Reimbursement Guidelines
- Understand Medicare Policy on Power Mobility Devices



