Table of Contents
- Understanding Medicare Coverage for Power Wheelchairs
- Medicare Eligibility and Coverage Criteria for Power Wheelchairs
- Documentation and Prior Authorization for Power Wheelchair Medicare
- Clinical Evaluations and Model Selection for Medicare Power Wheelchairs
- Processing Timelines, Appeals, and Support for Power Wheelchair Medicare
- Frequently Asked Questions on Power Wheelchair Medicare
- Your Path to Medicare-Funded Power Mobility
Understanding Medicare Coverage for Power Wheelchairs
Navigating power wheelchair medicare coverage can feel overwhelming, but we’re here to simplify it for you. As a key part of Medicare’s durable medical equipment benefits, power wheelchairs provide essential mobility for those with significant limitations. Unlike manual wheelchairs, which rely on self-propulsion, power wheelchairs use motors and batteries for independent movement, as defined by the Centers for Medicare & Medicaid Services (CMS). This distinction ensures coverage aligns with your specific needs in the United States.
To qualify under medicare power wheelchair coverage criteria, medical necessity must be established. According to CMS, authoritative government health data, patients must demonstrate an inability to self-propel a manual wheelchair due to conditions like severe arthritis or neurological disorders. A face-to-face physician evaluation is required, along with a written order prior to delivery. Key requirements include:
- Inability to perform mobility-related activities of daily living within the home.
- Need for power mobility to move safely and independently indoors.
- Improvement in functional abilities not achievable with alternatives.
For power wheelchair medicare prior authorization, your doctor certifies necessity using the Medicare Power Mobility Device Checklist, while the DME supplier submits Form CMS-10126. Coverage limits include one power wheelchair every five years, emphasizing compliant choices.
Common accessories like batteries, chargers, and seating systems are often covered if reasonable and necessary. Medicare wheelchair options coverage details allowable items, such as heavy-duty options with HCPCS code E2371, while advising against non-standard cushions per CMS compliance guidelines. As your partner in mobility freedom, we handle the paperwork, insurance navigation, and coordination to secure these benefits efficiently.
To verify your coverage, contact your Medicare plan or a local DME provider like us in Spring Valley, NY. This ensures smooth access—next, learn how to select a compliant supplier for seamless delivery.
Medicare Eligibility and Coverage Criteria for Power Wheelchairs
Building on the advantages of power wheelchairs, understanding Medicare coverage is crucial for eligible users. If you’re exploring power wheelchair medicare options, know that beneficiaries must have Medicare Part B coverage and face a mobility impairment that limits daily activities, such as walking or household tasks. This ensures the device addresses real needs rather than conveniences. We at MedEquipped guide patients through these steps, helping confirm if a power wheelchair fits your situation.
Medicare requires a face-to-face physician examination to document why you cannot effectively use a cane, walker, or manual wheelchair. The doctor must detail your condition, like arthritis or neurological issues, and explain how it impacts mobility inside the home. According to the Centers for Medicare & Medicaid Services (CMS), this exam forms the foundation for approval, proving the device is medically necessary.
Next comes the home assessment, which evaluates if the power wheelchair is reasonable for your living space. It must improve navigation in rooms and hallways without excessive space demands. Centers for Medicare & Medicaid Services (CMS) guidelines stress that coverage focuses on home use, not outdoor adventures. We handle these assessments as part of our service, ensuring everything aligns with requirements.
When detailing documentation, power wheelchair medicare prior authorization becomes key, especially for advanced models. You’ll need a standard written order from your physician, plus supporting records like therapy notes. For Groups 2 and 3, prior authorization often applies, requiring detailed justification. MedEquipped, as industry supplier guidance, explains that common denials stem from incomplete paperwork, which we help resolve.
Medicare classifies power wheelchairs into three groups under medicare power wheelchair coverage criteria, based on your mobility needs and required features. Group 1 suits basic indoor use for mild to moderate impairments, with speeds up to 3.6 mph and no tilt or recline. Group 2 offers versatility for indoor and outdoor mobility, ideal for moderate needs with programmable controls and better obstacle handling. Options like foldable electric wheelchairs fit here, providing portability for users facing environmental barriers. Group 3 addresses severe limitations with custom seating, power tilt or recline, and heavy-duty bases like the TDX SP2 HD.
These groups require escalating documentation: Group 1 needs proof a manual chair won’t suffice, while Groups 2 and 3 demand an Assistive Technology Professional (ATP) evaluation. Centers for Medicare & Medicaid Services (CMS) Local Coverage Determination (LCD) outlines these, including prior authorization for higher groups. Upcoming 2026 updates will stress stronger clinical justification and records.
The following table summarizes Medicare’s group levels for power wheelchairs:
Medicare Group Coverage Levels for Power Wheelchairs
This table compares Medicare’s group classifications for power wheelchairs based on mobility needs and features.
| Group Level | Mobility Impairment Description | Key Features Covered | Medicare Criteria Highlights |
|---|---|---|---|
| Group 1 | Mild to moderate impairments | Basic controls, no tilt or recline | Requires face-to-face exam and home assessment |
| Group 2 | Moderate impairments requiring more support | Tilt or recline options, programmable controls | Needs detailed medical documentation |
| Group 3 | Severe mobility limitations | Custom seating, power tilt/recline, standing features | Prior authorization often required |
Data sourced from CMS Local Coverage Determination (LCD) for Power Mobility Devices. This visual breakdown helps clarify how each group matches specific impairments and features, making it easier to identify what Medicare might cover for your needs.
Reviewing these criteria shows how Medicare tailors coverage to individual challenges, from basic mobility aids to advanced custom setups. If a claim faces denial due to insufficient documentation, appeal by submitting additional evidence like updated physician notes or ATP reports. Suppliers like us at MedEquipped play a key role in this process, offering guidance on resubmissions. Once eligibility is confirmed, the next phase involves gathering documentation for approval.
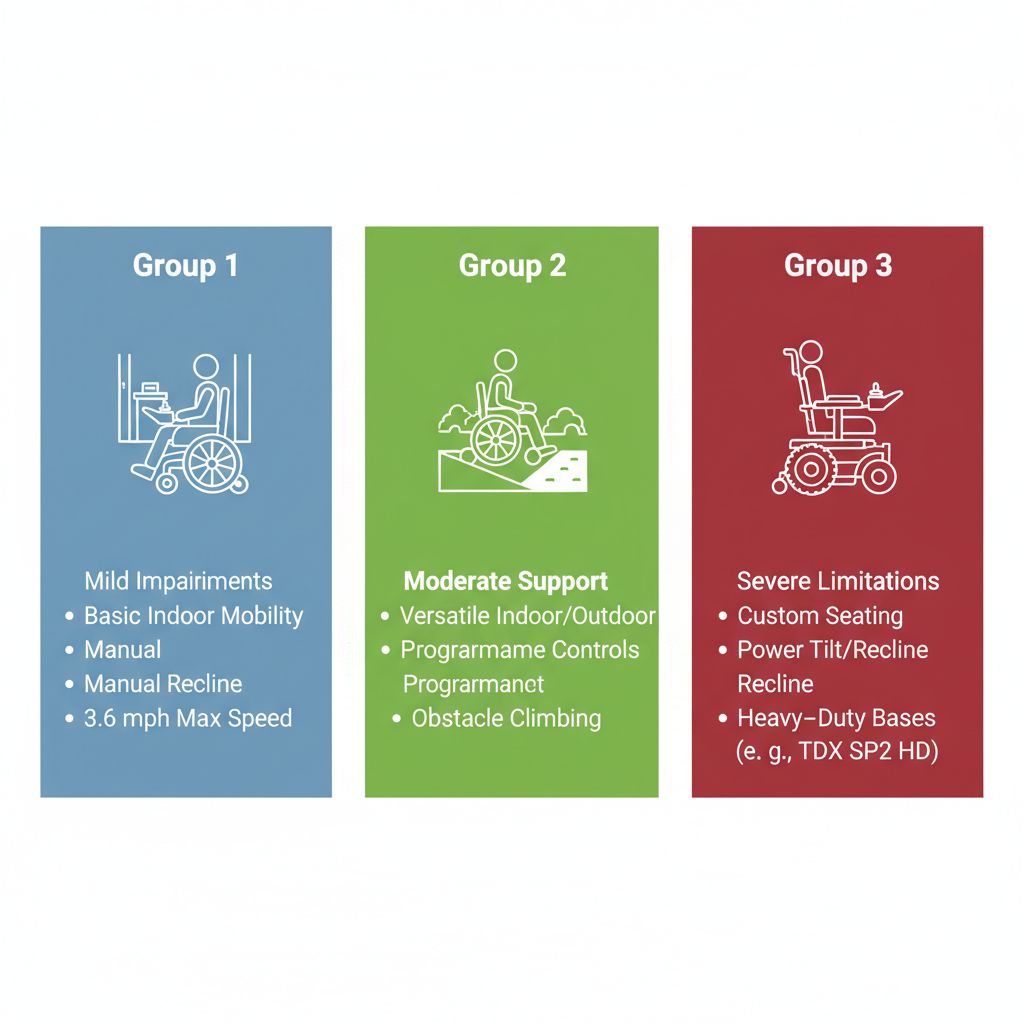
Comparison of Medicare power wheelchair groups by coverage and features
This infographic reinforces the group distinctions, highlighting how features align with impairment levels to meet Medicare standards effectively.
Documentation and Prior Authorization for Power Wheelchair Medicare
Once eligibility is established, the next critical step involves gathering documentation and securing prior authorization for power wheelchair medicare. At MedEquipped, we understand how overwhelming this can feel, so we handle the paperwork, insurance navigation, and coordination to make the process smoother for you. This ensures your custom motorized wheelchair arrives as a true partner in mobility freedom.
Required Medical Documentation for Approval
To meet medicare power wheelchair coverage criteria, your physician must provide detailed evidence showing why a power wheelchair is medically necessary over a manual one. This includes documenting severe mobility limitations that prevent safe use of a cane, walker, or manual wheelchair. According to practical FAQ guidance from MedEquipped, a supplier like us can help compile these materials to avoid delays.
Key requirements include:
- Form CMS-10126 (Supplier Statement): Completed by your doctor and the supplier, outlining the wheelchair’s specifications and confirming it meets your needs.
- Physician office notes: These should describe your functional limitations, such as inability to stand or walk more than a short distance without assistance, with specific examples of daily challenges.
- Face-to-face examination report: An in-person doctor visit within the last 6 months, including a written order justifying the power mobility device.
Additionally, assessments from a certified Assistive Technology Professional (ATP) can strengthen your case, especially for complex needs. For instance, common denial reasons like insufficient functional goals can be mitigated with an ATP evaluation that details how the wheelchair supports independence. This thorough documentation aligns with Medicare’s standards, helping ensure approval for devices like the TDX SP2 HD or QUICKIE series.
Navigating the Prior Authorization Process
Securing power wheelchair medicare prior authorization involves a structured submission to verify compliance before delivery. We at MedEquipped guide you every step, leveraging our expertise in Medicare processes across New York, Georgia, and Michigan. This end-to-end support typically wraps up in our 30-60 day faster processing timeline.
Follow these steps for a successful request:
- Physician completes the DME Medical Documentation form: Gather the face-to-face exam, written order, and supporting notes as outlined earlier. Ensure everything highlights medical necessity under Medicare Part B.
- Supplier submits via myCGS portal: As your supplier, we upload all documents with the appropriate HCPCS code. The Medicare DME prior authorization process requires this electronic submission for items on the Required Prior Authorization List, as outlined by the Centers for Medicare & Medicaid Services.
- Track status on CMS portal: Provisional affirmation can occur quickly if initial docs are complete, with standard reviews now at seven calendar days per recent CMS updates. Log in regularly or let us monitor for you.
- Appeal denials within 120 days: If needed, use the specific appeal form with additional evidence, such as an ATP report addressing gaps like terrain needs or weight capacity.
Certain HCPCS codes for power wheelchairs trigger these requirements, focusing on high-utilization items to protect Medicare resources. The table below compares common codes and notes, based on CMS prior authorization initiatives for DME.
| HCPCS Code | Wheelchair Type | Prior Auth Required? | Key Documentation Notes |
|---|---|---|---|
| K0005 | Heavy-duty power wheelchair | Yes | Detailed clinical justification for weight and terrain |
| E2372 | Group 3 power base | Yes | Home assessment and functional goals |
This comparison helps identify what extra steps your claim might need, reducing surprises. For example, heavy-duty models like K0005 often require proof of bariatric needs, while Group 3 bases demand evidence of postural support requirements. Supplier-provided procedural advice from MedEquipped emphasizes including these details upfront to boost approval rates.
To avoid denials from vague functional goals, always tie documentation to real-life impacts, like navigating home obstacles. On average, non-urgent requests process in 10-14 days, though expedited reviews for imminent health risks can shorten this to two business days per CMS guidelines. With approval in hand, identifying the right supplier ensures seamless delivery and customization.
Clinical Evaluations and Model Selection for Medicare Power Wheelchairs
The Role of Certified ATP Evaluations
Our certified Assistive Technology Professionals (ATPs) play a vital role in Medicare power wheelchair evaluations. We start by conducting thorough mobility assessments to understand each patient’s unique challenges. Using standardized tools like the Wheelchair Skills Test, we evaluate how well someone navigates their home and community. This step identifies functional limitations, such as difficulty with transfers or endurance, ensuring recommendations match real-life demands.
For patients upgrading from manual wheelchairs to power options, we contrast basic manual mobility with advanced power systems. Medicare power wheelchair coverage criteria require detailed documentation, including a physician’s prescription outlining medical necessity and reports on functional impairments. We handle the paperwork, insurance navigation, and coordination to simplify this for you. Our ATPs then recommend custom features, like power tilt for pressure relief, based on clinical justification from the evaluation.
These assessments comply with RESNA standards, focusing on safety and comfort. According to MedEquipped’s internal FAQ guidance on professional assessment standards under Medicare guidelines, this comprehensive approach ensures eligibility and optimal outcomes. We emphasize patient involvement, discussing goals to build confidence in the selected device.
Selecting Medicare-Covered Models Like QUICKIE and ROVI X3
Choosing the right Medicare-covered power wheelchair involves understanding Group classifications and features that meet your needs. In 2026, we focus on models like the QUICKIE Series and ROVI X3, which offer robust compliance with Centers for Medicare & Medicaid Services (CMS) rules. Our team at MedEquipped helps navigate these options, ensuring selections support indoor and outdoor use while addressing specific impairments.
Medicare divides power wheelchairs into Group 2 for moderate needs, allowing indoor/outdoor mobility with speeds up to 4 mph, and Group 3 for more complex rehab scenarios, featuring higher speeds up to 6 mph and greater weight capacities up to 300 pounds or more. Group 2 suits those with moderate impairments requiring versatile navigation, while Group 3 handles severe mobility challenges, like navigating uneven terrain or home barriers. As your partner in mobility freedom, we explain these differences during consultations to match the best fit.
Custom features, such as power tilt, recline, or programmable controls, require power wheelchair medicare prior authorization, including clinical notes justifying medical necessity under complex rehab tech criteria. For instance, sling seat authorization needs proof of skin integrity risks, and we coordinate these approvals seamlessly. MedEquipped’s internal FAQ on coverage rules highlights that prior auth ensures features like heavy-duty bases are Medicare-eligible, preventing claim denials.
Popular models vary by these classifications, as shown in the comparison below. Sourced from MedEquipped product FAQs and CMS coverage rules, this table outlines key differences to aid your decision:
| Model | Group Classification | Key Medicare-Covered Features | Best For |
|---|---|---|---|
| QUICKIE Series | Group 2/3 | Custom seating, power tilt | Moderate to severe impairments |
| ROVI X3 | Group 3 | Heavy-duty base, recline options | Severe mobility needs |
| TDX SP2 HD | Group 3 | Extra stability, programmable controls | ALS/MS patients |
The QUICKIE Series excels for versatile daily use, while the ROVI X3 and TDX SP2 HD provide advanced stability for demanding conditions. We deliver these custom motorized wheelchairs in 30-60 days, faster than many providers, with full setup and education.
Once evaluated and a model selected, proceed to prior authorization steps for seamless access to your Medicare benefits.
Processing Timelines, Appeals, and Support for Power Wheelchair Medicare
Once eligibility under medicare power wheelchair coverage criteria is established, the next phase involves navigating processing timelines for power wheelchair Medicare approval. We at MedEquipped understand that waiting for your custom motorized wheelchair can feel daunting, but the overall process typically spans 30-60 days from application to delivery. Factors like complete documentation and prompt submissions can speed things up, helping you get back to greater mobility sooner. As your partner in mobility freedom, we handle the paperwork, insurance navigation, and coordination to make this smoother.
The first stage is prior authorization for your power wheelchair Medicare request. This involves submitting necessary medical necessity documents through the Durable Medical Equipment Medicare Administrative Contractor (DME MAC), a regional Medicare reviewer that handles claims. According to practical, experience-based timelines from MedEquipped, this review usually takes 10-14 days. We emphasize power wheelchair Medicare prior authorization early to avoid delays, and in Michigan, state assistance often accelerates this step.
Following prior authorization, the clinical evaluation and order stage begins, lasting 7-21 days. Here, a certified Assistive Technology Professional (ATP) conducts an assessment to configure your chair for optimal fit and function, including custom seating and controls. MedEquipped’s New York office streamlines this process, aiming for the full 30-60 day timeline overall. This personalized fitting ensures your power wheelchair meets Medicare coverage for power wheelchairs standards while suiting your daily needs.
Finally, approval and delivery wrap up the process within the total 30-60 days. Once approved, we manage insurance billing and ship your fully fitted chair directly to you, followed by post-delivery adjustments and education. Local support in Georgia and Michigan enhances this, providing hands-on guidance for seamless integration into your routine. These faster processing timelines set us apart, often quicker than national averages.
The following table outlines the Medicare Power Wheelchair Processing Stages, providing a timeline comparison across stages from application to delivery, derived from CMS guidelines and MedEquipped timelines.
| Stage | Typical Duration | Key Actions | Regional Variations (NY/GA/MI) |
|---|---|---|---|
| Prior Authorization | 10-14 days | Submit docs via DME MAC | Faster in MI with state assistance |
| Clinical Evaluation & Order | 7-21 days | ATP assessment and config | NY office streamlines |
| Approval & Delivery | 30-60 days total | Insurance billing, ship fitted chair | GA/MI local support |
This breakdown highlights how regional factors influence power wheelchair Medicare speeds. For instance, New York’s efficient evaluations and Michigan’s aid can shorten waits compared to standard processes.
If delays or denials occur in your power wheelchair Medicare journey, appeals provide a clear pathway forward. Denials can be frustrating, but structured appeals often succeed with our guidance. Key steps include:
- Request a redetermination within 120 days of the denial notice, submitting additional evidence of medical necessity.
- If unsatisfied, escalate to a Qualified Independent Contractor review, then an Administrative Law Judge (ALJ) hearing for further adjudication.
We recommend acting quickly to preserve your options.
For support, MedEquipped coordinates every application aspect across New York, Georgia, and Michigan. In Michigan, the State Health Insurance Assistance Program (SHIP), an official resource from the Michigan Department of Health and Human Services, offers free counseling on Medicare appeals and timelines. Contact them or us at 845-237-2381 for personalized help. If power wheelchair approval is denied, exploring options like manual wheelchairs may provide interim mobility solutions. After approval and delivery, ongoing support ensures optimal use—see our post-delivery care guide.
Frequently Asked Questions on Power Wheelchair Medicare
To further clarify coverage details on power wheelchair Medicare, here are answers to common questions. At MedEquipped, we guide patients through these processes as your partner in mobility freedom.
What are the eligibility requirements for power wheelchair Medicare?
Medicare guidelines for power wheelchair eligibility require functional mobility limitations, like inability to self-propel a manual wheelchair, confirmed by a physician’s assessment as authoritative government health data from the Centers for Medicare & Medicaid Services indicates.
What documentation meets Medicare power wheelchair coverage criteria?
Coverage needs proof of medical necessity, including a physician prescription, face-to-face evaluation, and home assessment showing the wheelchair’s essential role in daily activities within Medicare power wheelchair coverage criteria.
How does the power wheelchair Medicare prior authorization process work?
Suppliers submit claims through Medicare’s DMEPOS system with supporting documents like the Written Order Prior to Delivery; we handle the paperwork, insurance navigation, and coordination in power wheelchair Medicare prior authorization processes.
What are key compliance tips for Medicare wheelchair options?
Use proper HCPCS E codes for billing, avoid non-covered recreational accessories, and apply modifiers like KX for claims. For more, see Medicare wheelchair compliance tips.
This is general information; consult CMS resources or a professional for personalized advice. Information is not medical advice and is for informational purposes only. For help starting your claim, see the following guide.
Your Path to Medicare-Funded Power Mobility
Building on basic coverage details, gaining Medicare-funded power mobility can transform daily life for those with limited mobility. At MedEquipped, we guide you through obtaining a power wheelchair medicare device, covering 80% after your deductible for eligible needs.
Eligibility Check: Start with a doctor’s visit to confirm medicare power wheelchair coverage criteria, like arthritis or neurological issues requiring a prescription for medical necessity.
Application Process: Gather a face-to-face exam summary, supplier form, and home proof if needed. We handle power wheelchair medicare prior authorization as your DME partner, submitting claims efficiently.
Contact us at 845-237-2381 for free consultations and fittings. We handle the paperwork, insurance navigation, and coordination. Once approved, explore models that fit your needs for true mobility freedom.
This article was researched and written with the assistance of AI tools.
Resources
- Discover Custom Motorized Wheelchairs for Enhanced Mobility
- Find Lightweight QUICKIE Manual Wheelchairs for Easy Portability
- Get Custom Manual Wheelchair Solutions for Independence
- Locate Orthotics Providers for Power Wheelchair Customization
- Schedule RESNA-Certified Wheelchair Fitting Services in Georgia
- Access Custom Orthotics and Mobility Evaluations in Key States
- Learn Mobility Solutions and Customized Wheelchair Access Guidance
- Explore Medicare Coverage Rules for Wheelchair Options
- Obtain CMS Compliance Tips for Wheelchair Accessories Billing
- Understand Medicare Prior Authorization Process for DMEPOS Items
- Review Medicare Criteria for Power Mobility Device Coverage
- Access Free Michigan SHIP Medicare Assistance Program